Heel pain is a common symptom that has many possible causes. Although heel pain is sometimes caused by a systemic (body-wide) illness, such as rheumatoid arthritis or gout, it is usually a local condition that affects only the foot. The most common local causes of heel pain include:
Stone Bruise
When you step on a hard object such as a rock or stone, you can bruise the fat pad at the bottom of your heel. It may or may not look discolored. The pain goes away gradually with rest.
Plantar Fasciitis
Doing too much running or jumping can inflame the tissue band (fascia) joining the heel bone to the base of the toes. The pain is centered under your heel and may be mild at first, but flares up when you take your first steps after recuperating overnight. You may need to do special exercises, take medication to reduce the swelling and use a heel pad in your shoe.
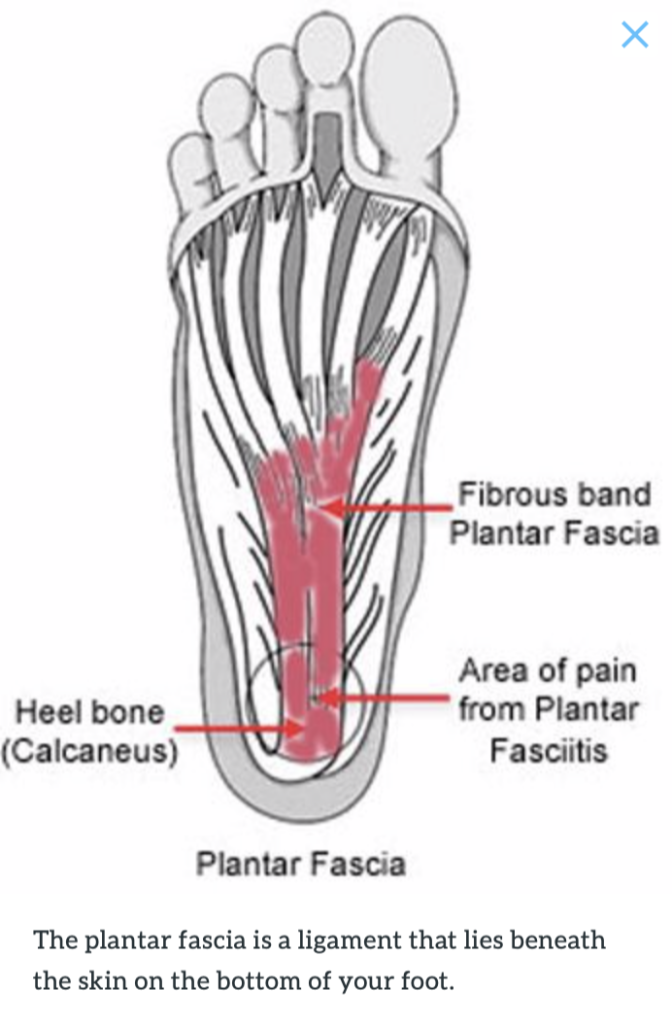
Heel Spur
When plantar fasciitis lasts for a long time, a heel spur (calcium deposit) may grow where the fascia tissue band attaches to your heel bone. Your doctor may take an X-ray to see the bony protrusion, which can range in size. Therapy is habitually the same as for plantar fasciitis: rest until the pain subsides, do special stretching exercises and wear heel pad shoe inserts.
Calcaneal Apophysitis
In this condition, the center of the heel bone becomes irritated as a result of a new shoe or increased athletic activity. This pain occurs in the back of the heel, not the bottom. Calcaneal apophysitis is a moderately common cause of heel pain in active, growing children between the ages of 8 and 14. Although nearly any boy or girl can be affected, children who participate in sports that require a lot of jumping have are at the highest risk of developing this condition.
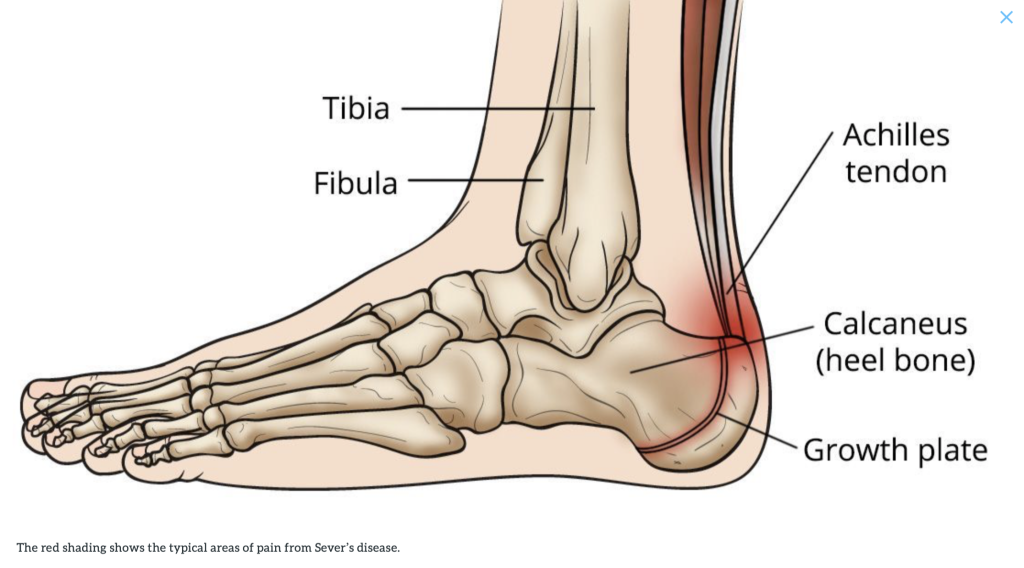
Bursitis
Bursitis means inflammation of a bursa, a sac that lines many joints and allows tendons and muscles to move easily when the joint is moving. In the heel, bursitis may produce pain at the underside or back of the heel. In some cases, heel bursitis is linked to structural problems of the foot that cause an irregular gait (way of walking). In other cases, wearing shoes with inadequately cushioned heels can trigger bursitis.
In Part 2 of this article about common heel pain causes, we will present to you the other five conditions responsible for heel pain. Stay tuned!
When to Call the Doctor
If you are unsure of the cause of your symptoms, or if you do not know the specific treatment recommendations for your condition, seek medical attention.
If you have suffered from heel pain, it’s almost impossible to diagnose yourself. There are many conditions with very similar symptoms. So the best thing you can do is visit a foot and ankle specialists in Cary or a location convenient for you to get medical advice and consultation.
Here are some definite signs that you should be evaluated by a doctor:
- Inability to walk comfortably on the affected side
- Heel pain that occurs at night or while resting
- Heel pain that persists beyond a few days
- Swelling or discoloration of the back of the foot
- Signs of an infection, including fever, redness, and warmth
- Any other unusual symptoms
Foot and Ankle Care at Raleigh Orthopaedic
The Raleigh Orthopaedic Clinic’s board-certified, fellowship-trained foot and ankle specialists bring together many years of experience to diagnose, manage and correct various foot conditions. These include, but are not limited to: bunions, hammertoes, mechanical imbalances of the feet, sprains and strains, fractures, arch pain, arthritis or warts.
Raleigh Orthopaedic Clinic’s Board Certified Podiatrist, Dr. Carroll Kratzer, works closely with our foot and ankle surgeons, Dr. David Boone and Dr. Kevin Logel, to provide patients with conservative treatment options, performing in-office procedures, if necessary.
Find your nearest Raleigh Orthopaedic clinic to get specialized treatment with a personal approach. Our team is happy to answer any questions or concerns you have.
Other articles that may interest you:
Choosing Shoes for a Fall-Free Life [6 Simple Tips for Older People]
The material contained on this site is for informational purposes only and DOES NOT CONSTITUTE THE PROVIDING OF MEDICAL ADVICE, and is not intended to be a substitute for independent professional medical judgment, advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare providers with any questions or concerns you may have regarding your health.