Diagnosis and Treatment of Spinal Fractures in Wake County

What is a Spinal Fracture?
A spinal fracture or dislocation of one or more vertebrae in the spine can cause bone fragments to pinch, damaging the spinal cord or surrounding nerves. Most spinal fractures occur because of a high velocity accident and can involve the neck (cervical), mid-back (thoracic), or lower back (lumbar). A spinal fracture is considered a serious orthopedic injury, associated with trauma from motor vehicle accidents, a fall from a height, or a sports injury. Depending on the severity of your injury, you may experience moderate to severe pain, difficulty walking, or the inability to move your arms or legs (paralysis). Many fractures can heal with conservative treatment; however, surgery is sometimes required to realign the bones.

What Causes a Spinal Fracture?
Spinal fractures can occur due to a variety of factors. When an external force is applied to the spine, excess pressure is placed on the bones within the vertebral column. This may cause the front part of the vertebral body to crush, resulting in a compression fracture. If the entire vertebral column breaks, it is known as a burst fracture. Other risk factors related to fractures include cancer and osteoporosis, a disease which causes the bones to weaken over time.
Spinal Fracture Risk Factors
Most people’s risk factors for spinal injury increase as they age. This is especially true for women, due to their increased risk of osteoporosis. Additional risk factors for spinal fractures include:
- Caucasian/Asian race
- Age over 50
- Experiencing early menopause
- Slim or underweight build
- Smoking
- Cancer that has spread through the bones
Symptoms of a Spinal Fracture
Symptoms of a spinal fracture will vary depending on the severity and location of the injury. A fracture of the thoracic or lumbar spine causes mild to severe back pain that worsens with movement. If the spinal cord or nerves are involved, the patient may experience:
- Numbness
- Tingling
- Weakness in the limbs
- Muscle spasms
- Bowel/bladder dysfunction

Types of Spinal Fracture Patterns
There are 3 major types of spine fracture patterns: Flexion, Extension, and Rotation. Raleigh Orthopaedic spine specialists in NC classify fractures of the thoracic and lumbar spine based on a specific pattern of the fracture and whether there is a spinal cord injury. This classification helps determine the proper treatment for the spinal fracture.
The flexion fracture pattern includes both compression and axial burst fractures. With a compression fracture, the front (anterior) of the vertebra breaks and loses height, while the back (posterior) part of it does not. This type of fracture is usually stable – the bones have not moved out of place – and is rarely associated with neurological problems. With an axial burst fracture, the vertebra loses height on both the front and back sides, and can sometimes result in nerve compression. Some are stable, while others are significantly unstable.
A flexion/distraction (chance) fracture is characterized by the extension fracture pattern. In this type of fracture, the vertebrae are pulled apart, causing what is considered to be an unstable fracture. A chance fracture can occur in a head-on car collision when the upper body is thrown forward while the pelvis is stabilized.
The rotation fracture pattern includes the transverse process fracture and fracture-dislocation. Transverse process fractures result from rotation or extreme sideways (lateral) bending. However, they are uncommon and seldom affect stability. A fracture-dislocation involves the bone and/or soft tissue in which a vertebra moves off an adjacent vertebra. This injury frequently causes spinal cord compression.
How is a Spinal Fracture Diagnosed?
Vertebral fractures are diagnosed via X-ray in the respective location of the spine – neck, mid back, or low back. Then, your orthopedic specialist will generally order a CT scan to visualize any changes in the bone structure. In some instances, an MRI may also be performed to evaluate the surrounding soft tissues, ligaments, and intervertebral discs, or to identify an injury.
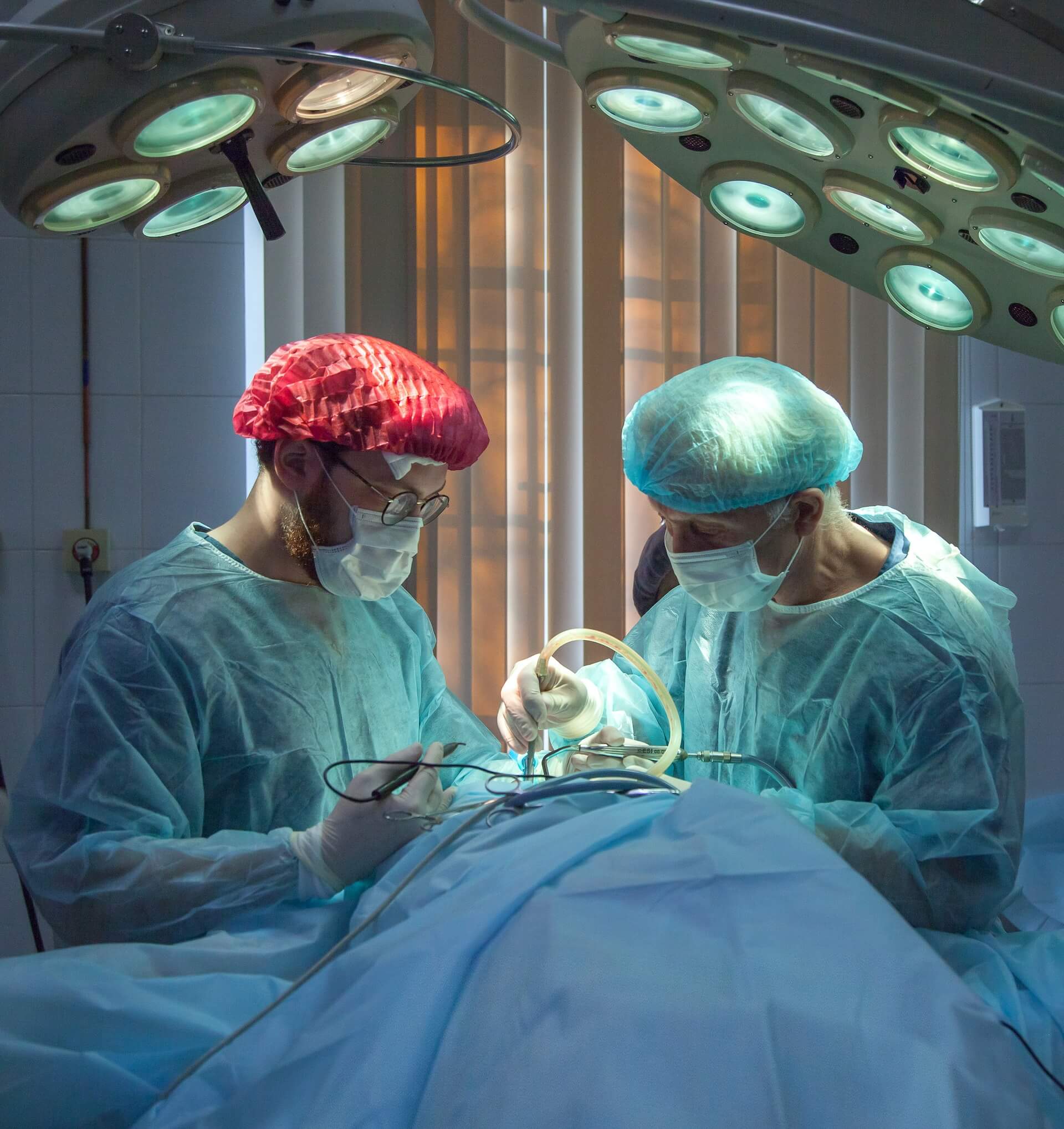
Treatment for Spinal Fractures in NC
Treatment for spinal fractures usually begins with pain management and stabilization to prevent further injury. Most minor fractures can be treated with cervical bracing to maintain spinal alignment, immobilize the spine during healing, and control the pain by restricting movement. After about 8 to 12 weeks, the brace can be removed.
More complex fractures or fractures with spinal cord compression may require surgery to ensure proper healing. The goal of surgery is to fuse and repair the fractured vertebrae, eliminate back pain, and restore posture and ease of movement. The most common surgical treatment options for spinal fractures are lumbar fusion and vertebroplasty/kyphoplasty. Lumbar fusion is a minimally-invasive procedure that joins the bones of the lower back using rods.
Vertebroplasty and kyphoplasty are more advanced, image-guided procedures performed in an X-ray suite or operating room with supporting X-ray equipment. In both of these surgeries, the neurosurgeon is able to reconstruct compressed vertebral bone, remove pressure on a nerve, and restore alignment.
Spinal Fracture Recovery Time
Regardless of whether a patient undergoes nonsurgical or surgical treatment, there will be a period of rehabilitation after the fracture has healed. For most spinal fractures, surgery is not needed and many patients respond well to conservative therapies such as bracing. Generally, you should avoid any intense physical activity for 12 weeks to allow the body to fully recover. Your doctor may recommend treatments to address bone density loss during this period and will carefully monitor the injury for any changes.
How Can I Prevent Neck and Back Fractures?
Accidents have the unfortunate quality of taking you by surprise. Natural ways to prevent spinal fractures include:
- Taking calcium supplements
- Taking vitamin D supplements
- Quitting smoking
- Doing weight-bearing and strength-building exercises
If you have or believe that you are at risk for osteoporosis, you can take medications to either slow or stop its effects – though you must consult with your physician beforehand.

Expert Neck and Back Care at Raleigh Orthopaedic
If you or a loved one has experienced a spinal fracture, look no further than Raleigh Orthopaedic for medical assistance and treatment. Our expert spine, neck, and back specialists diagnose and treat a wide range of spinal conditions and injuries. Contact us today and schedule an appointment at one of our convenient locations in Wake County, NC.

